Good health and well-being
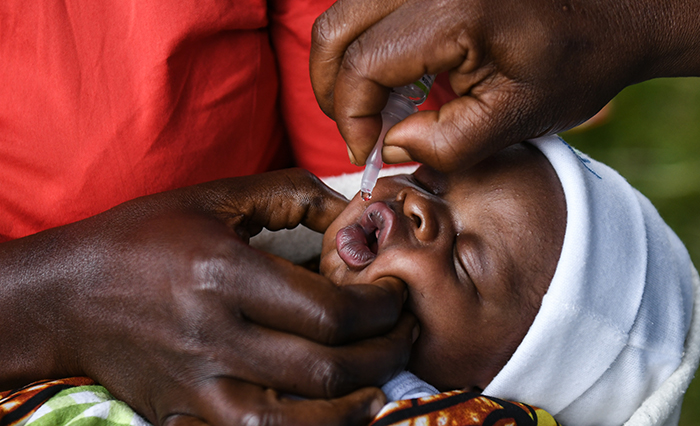
A child receives an oral polio vaccine during the launch of a nationwide polio campaign in Malawi.
© UNICEF/Thoko ChikondiThe COVID-19 pandemic turned back progress in life expectancy and gains in combating communicable diseases
The COVID-19 pandemic has significantly affected global health, reversing steady progress in life expectancy over the past two decades. Prior to the pandemic, global life expectancy rose consistently, from 66.8 years in 2000 to 73.1 years in 2019, reflecting years of improvements in health and related areas. COVID-19 swiftly reversed this positive trend, with global life expectancy plummeting to 71.4 years by 2021, back to the level of 2012.
Before the pandemic, non-communicable diseases had been steadily increasing as the leading cause of death, accounting for 59.5 per cent of all deaths in 2000 and 73.9 per cent in 2019. The share of communicable diseases dropped from 32.2 per cent in 2000 to 18.2 per cent in 2019. As COVID-19 emerged as a new infectious disease and started to take a toll on human lives, the share of deaths due to communicable diseases jumped back to the 2005 level (28.1 per cent) in 2021, while the share of deaths due to non-communicable diseases decreased to 65.3 per cent. COVID-19 ranked among the top three leading causes of death globally in 2020 and 2021, with striking regional variations.
Progress towards universal health coverage has slowed, leaving billions without care and subject to catastrophic costs
Essential health service coverage is measured using an index, reported on a score of 0 to 100, based on 14 indicators across four domains: reproductive, maternal, newborn and child health; infectious diseases; non-communicable diseases; and service capacity and access. The global score on the index increased remarkably from 45 in 2000 to 65 in 2015. Progress slowed thereafter, however, reaching a score of only 68 in 2021. The proportion of the population lacking essential health services fell by approximately 15 per cent between 2000 and 2021. Yet minimal progress after 2015 left about 4.5 billion people without coverage in 2021, especially in rural and poorer populations.
Financial hardship due to out-of-pocket health spending has worsened since 2015, affecting 2 billion people in 2019. They included 1 billion people facing catastrophic health expenditures exceeding 10 per cent of their household budget and 344 million driven deeper into extreme poverty by health costs. The proportion of the population with catastrophic expenditures increased from 12.6 per cent in 2015 to 13.5 per cent in 2019.
An ageing health workforce struggles to meet rising demands from an ageing population
Progressing towards universal health coverage requires addressing the global shortage of health workers. Yet data from 2015 to 2022 reveal stark disparities, with low-income countries experiencing the lowest health worker density and distribution. Per 10,000 people, these countries had medians of only 1.1 medical doctors, 7.5 nursing and midwifery personnel, 0.04 dentists and 0.2 pharmacists, compared with medians in high-income countries of 35.6 medical doctors, 76.8 nursing and midwifery personnel, 7.0 dentists and 8.8 pharmacists.
Health systems are experiencing increased strains in catering to the mounting health needs of an ageing global population, more so because the health workforce itself is ageing. An estimated 1.8 million additional health workers are needed in 54 countries, primarily high-income ones, to replace retiring health professionals and maintain the current age-standardized density of health workers.
Share of countries with an ageing workforce, by health occupation, 2017‒2022 (percentage)

Note: A health workforce is considered “ageing” when the share of health workers aged 55 years and above exceeds that of health workers aged 35 years and below.
Declines in maternal mortality have stalled, with wide disparities by region and income
Between 2015 and 2020, the global maternal mortality ratio declined only marginally from 227 to 223 maternal deaths per 100,000 live births, over three times higher than the 2030 target of 70. Sub-Saharan Africa and Southern Asia account for 87 per cent of maternal deaths. In 2020, the maternal mortality ratio in low-income countries was 430 maternal deaths per 100,000 live births compared to 13 in high-income nations. The average maternal mortality ratio for very high and high alert fragile states was 551 in 2020, more than twice the global average. Achieving the 2030 target requires an annual reduction rate of 11.6 per cent between 2021 and 2030.
Skilled birth attendance has improved globally, rising from 80 per cent of births in 2015 to 86 per cent in 2023. Improved care quality could save the lives of up to 1 million newborns and 150,000 mothers annually. Yet progress is stalling; 18 million births occurred without skilled assistance in 2023. In sub-Saharan Africa, only 73 per cent of births were attended by skilled personnel in 2023, the lowest rate worldwide. In contrast, Eastern and South-Eastern Asia achieved a rate of 96 per cent.
Improvements in adolescent birth rates and access to modern contraceptives do not benefit all women and girls equally
The adolescent birth rate for women aged 15‒19 years declined to 41.3 births per 1,000 women in 2023, from 47.2 in 2015 and 64.5 in 2000. For girls aged 10‒14 years, the rate fell from 3.3 births per 1,000 girls in 2000 to 1.8 in 2015 and 1.5 in 2023. Yet 13.1 million babies, approximately 10 per cent of the total number of births, were born to adolescent mothers in 2023. Central and Southern Asia witnessed the largest drop-offs in adolescent birth rates between 2000 and 2023, with a 72 per cent reduction in the 15-19 age group and a 90 per cent decrease in the 10‒14 cohort. Sub-Saharan Africa continued to have the highest rates globally, at 97.9 births per 1,000 women aged 15‒19 and 4.4 per 1,000 girls aged 10‒14 in 2023.
The proportion of women of reproductive age (15‒49 years) who have their need for family planning satisfied with modern methods has climbed from 76.5 per cent in 2015 to 77.6 per cent in 2024, corresponding to an additional 75 million women using modern contraceptive methods globally. By 2030, this proportion is projected to reach 78.2 per cent, a net increase of 45 million women. This marks a fair improvement but still falls far short of universal access.
Adolescent birth rate, by age group, 2000 and 2023 (births per 1,000 women or girls in each age group)

*Excluding Australia and New Zealand.
Under-5 deaths hit a record low in 2022; achieving the SDG target could save 9 million lives by 2030
Global under-5 deaths reached a historic low of 4.9 million in 2022, down from 9.9 million in 2000 and 6.0 million in 2015. Nearly half these deaths (2.3 million) occurred during the neonatal period (the first 28 days of life). The under-5 mortality rate was 37 deaths per 1,000 live births in 2022, a 51 per cent reduction since 2000 and a 14 per cent reduction from 2015. The global neonatal mortality rate fell to 17 deaths per 1,000 live births in 2022, a 44 per cent reduction since 2000 and a 12 per cent reduction since 2015.
Unfortunately, the annual rate of reduction in under-5 mortality contracted from 3.8 per cent in 2000‒2015 to 2.1 per cent in 2015-2022. The neonatal mortality rate followed a similar pattern, declining from 3.0 per cent to 1.8 per cent. If current trends continue, an estimated 35 million children will die before reaching their fifth birthday by 2030. If all countries met the target for under-5 mortality, an estimated 9 million lives could be saved by 2030. As of 2022, 134 countries had already met the target. Seven more were on track but 59 countries, nearly three quarters of which are in sub-Saharan Africa, will need faster progress to meet the target.
Under-5 and neonatal mortality rate, 2015‒2022 (deaths per 1,000 live births)

*Excluding Australia and New Zealand.
Efforts to combat communicable diseases have prevented millions of deaths but are threatened by inequalities and emerging threats
HIV/AIDS: The world has made significant strides in combating HIV. In 2022, an estimated 1.3 million new infections represented a 27 per cent decrease since 2015 and a 38 per cent reduction since 2010. Sub-Saharan Africa, the region most affected by HIV, has more than halved new infections annually since 2010. In 2022, 29.8 million of the 39 million people living with HIV were receiving life-saving treatment. Increased access to treatment has averted 20.8 million AIDS-related deaths in the past three decades. In addition, the integration of HIV testing and treatment with maternal and childcare services has prevented over 3.4 million HIV infections in children since 2000. Stronger linking of services for HIV and tuberculosis has averted an estimated 6.4 million tuberculosis-related deaths among people living with HIV from 2010 to 2022.
Not everyone is benefiting equally from these advancements, however. In 2022, 43 per cent of the 1.5 million children living with HIV were not receiving treatment. Every week, 4,000 adolescent girls and young women acquired HIV; 3,100 lived in sub-Saharan Africa. Almost a quarter of new HIV infections were in Asia in 2022. Steep increases of new HIV infections have continued in Northern Africa and Western Asia. These worrying trends are primarily due to a lack of preventive services for people from marginalized and key populations, punitive laws, violence, social stigma and discrimination.
HIV incidence rate, 2010 and 2022 (number of new infections per 1,000 uninfected adults aged 15‒49 years)

Tuberculosis: The reported number of people newly diagnosed with tuberculosis reached 7.5 million in 2022, the highest figure since global monitoring began in 1995 and above the previous historical peak of 7.1 million in 2019. Worldwide, an estimated 10.6 million people developed tuberculosis in 2022, up from 10.3 million in 2021 and 10.0 million in 2020. The disease remains the world’s second leading cause of death from a single infectious agent, with an estimated 1.3 million deaths in 2022. This was down from the estimated 1.4 million deaths in both 2020 and 2021 and almost back to pre-pandemic levels. The global net decrease in tuberculosis-related deaths between 2015 and 2022, however, was 19 per cent, well below the target of a 75 per cent reduction by 2025. The estimated disease incidence rate was 133 new cases per 100,000 population in 2022, a fall of 8.7 per cent since 2015. A return to the pre-pandemic downward trend may occur in 2023 or 2024.
Tuberculosis estimated incidence rate and case notification rate, 2015‒2022 (new cases per 100,000 population per year)

Malaria: An estimated 249 million malaria cases occurred globally in 2022, 16 million more than in 2019 before the pandemic. The disease claimed an estimated 608,000 lives in 2022, an increase of 32,000 compared to 2019. Since 2015, insecticide-treated net use among young children and pregnant women in sub-Saharan Africa has stagnated at around 56 per cent. In 2022, an estimated 58 per cent of at-risk pregnant women did not receive the recommended preventive malaria therapy, and about one third of children with fever did not receive care from a health provider. Alongside disruptions caused by COVID-19, the global malaria response faces increasing threats, including drug and insecticide resistance, humanitarian crises, funding constraints, delays in programme implementation and climate change impacts. Despite these challenges, some important achievements sustain progress towards elimination in many countries with a low malaria burden, with 25 countries reporting fewer than 10 cases in 2022. Thirteen countries have been certified malaria-free since 2015.
Malaria case incidence, 2015‒2030 (cases per 1,000 population at risk)

Neglected tropical diseases:
In 2022, 1.6 billion people required treatment and care for neglected tropical diseases, a 26.1 per cent decline from 2010. The proportion of the population living in LDCs who required interventions for these diseases decreased from 79 per cent to 45 per cent during this period. As of December 2023, 50 countries, territories and areas had eliminated at least one neglected tropical disease, demonstrating the power of comprehensive interventions combining mass and individual treatment, vector control, veterinary public health and provision of safe water and sanitation.
Progress has not been fast enough to meet the target of reducing the global population requiring interventions for neglected tropical diseases by 90 per cent between 2010 and 2030. Achieving this target demands a renewed effort to scale up interventions, particularly in high-burden countries, many of which are LDCs.
Twenty-one million children missed out on lifesaving vaccines in 2022
Between 2000 and 2019, the proportion of children receiving three doses of the diphtheria, tetanus and pertussis (DTP3) vaccine rose from 72 to 86 per cent, then dipped to 81 per cent in 2021 before rebounding to 84 per cent in 2022. In 2022, 20.5 million children missed at least one routine vaccine and 14.3 million received no vaccines at all. Coverage of two doses of the measles vaccine and three doses of the pneumococcal conjugate vaccine increased in 2022, reaching 74 per cent and 60 per cent, respectively, following stagnation in 2020‒2021. Global coverage of the human papillomavirus (HPV) vaccine, critical for women’s and girls’ health, stood at only 15 per cent in 2022, despite 130 countries introducing it in their national immunization services by the end of the year.
Treatment reaches only marginal shares of people with drug and alcohol disorders
Newly available estimates reveal that globally, only about 1 in 11 individuals with drug use disorders received related treatment in 2022. Coverage decreased from 11 per cent to under 9 per cent between 2015 and 2022, and has notably decelerated in the Americas and Asia. Treatment coverage for women consistently lags behind that for men across all regions, with over 13 per cent of men receiving treatment compared to less than 6 per cent of women in 2022. Data on access to treatment for those with alcohol use disorders indicate a dire situation, with coverage ranging from 0.3 per cent to a maximum of 14 per cent in reporting countries. Considering that approximately 283 million people or 5 per cent of the adult population lives with alcohol use disorders, hundreds of millions are going without needed treatment and care.
More than 9 in 10 deaths caused by air pollution occur in lower- and middle-income countries
Particulate air pollution caused approximately 104 deaths per 100,000 people annually by 2019, despite a slight decrease in the global mortality rate attributed to household and ambient air pollution since 2010. Ninety-three per cent of the burden fell on low- and middle-income countries in 2019, primarily in Asia and Africa. Non-communicable diseases accounted for 85 per cent of air pollution-related deaths, while acute lower respiratory infections made up the remaining 15 per cent. Concerningly, 31 per cent of deaths from acute lower respiratory infections occurred in children under age 5.
Oceania (excluding Australia and New Zealand), sub-Saharan Africa and most of Asia have the highest mortality rates attributable to air pollution. This is largely due to significant exposure to air pollution in households, a large proportion of which rely on polluting fuels and technologies for cooking, lighting and heating. Health risks from household air pollution are particularly high among women and children, who tend to spend more time in and around cooking stoves.
Age-standardized mortality rate attributed to household and ambient air pollution, 2010-2019 (deaths per 100,000 population)

* Excluding Australia and New Zealand.
Official development assistance for health has scaled up but with a major share spent on COVID-19
Total net official development assistance (ODA) for medical research and basic health sectors has significantly increased in recent years, primarily driven by the global response to the COVID-19 pandemic. ODA for basic health care from all donors more than doubled in real terms between 2015 and 2022, rising from $10.5 billion to $21.1 billion (in constant 2022 prices). It rose 4.4 per cent in 2022 compared to 2021. In 2022, COVID-19 control constituted the largest share of ODA for basic health care at 42 per cent, totalling $8.8 billion, of which $1.6 billion was for COVID-19 vaccine donations. Between 2020 and 2022, COVID-19 control received $22.5 billion in total ODA. Other ODA expenditure in 2022 comprised $3.7 billion on infectious disease control, $2.4 billion on malaria control and $2.2 billion on basic health care. By region, sub-Saharan Africa received the largest volume and share of aid for basic health care, amounting to $6.6 billion.
Total official development assistance to medical research and basic health sectors, 2015-2022 (billions of constant 2022 US dollars)