(With contributions from: Aravinda Guntupali, Ana Amelia Camarano, Gabrielle Kelly, Ishtar Govia, Nadia Minicuci, Barbara Corso and Ilaria Rocco)
Global and national health agencies do not always include older people in the way they develop, apply and interpret data. For much of the HIV pandemic, data were not collected for people aged 50 or more, based on the misguided view that older people were not at risk of infection(1). More recently, older people have been excluded from mortality reporting and from WHO targets for non-communicable diseases (NCDs), such as heart disease and diabetes, even though they are disproportionately at risk of dying from these conditions(2). Has this bias changed during the COVID-19 pandemic, given the strong association between old age and risk of death?
This blog focusses on COVID-19 mortality data. The pandemic is generating many other direct and indirect effects beyond mortality, and many of them will vary across age groups. For example, there is evidence that older people are disproportionately affected by all-cause excess mortality, in part because they have a high burden of unmet health care needs for other conditions(3).
Neither of the two most widely-used COVID-19 databases (WHO’s COVID-19 dashboard and Johns Hopkins Coronavirus Resource Centre) currently provide age-specific data, and neither makes specific reference to this issue(4,5). Hopefully, this will change in the near future.
What about data for older people in low and middle-income countries (LMICs), the group most affected by COVID-19 mortality to date?(6). Table 1 presents what is currently available for the 12 LMICs reporting the largest number of COVID-19 deaths by 2 November 20201. Two of those 12 countries (Iran and Russia) are not included in the table, as they do not currently provide COVID-19 mortality data by ages. In a further three countries (Argentina, Ecuador and South Africa), no updated age-disaggregated data were published between June/July 2020 and the start of November 2020.
Table 1 shows that the share of reported COVID-19 deaths accounted for by people aged 60 or more ranged from 43% in Indonesia to 84% in Chile. This variation is in part a consequence of national population age structures: in 2020, 10.1% of Indonesia’s population was aged 60 or more, compared to 17.4% of Chile’s(7). However, the relationship between age structure and age composition of COVID-19 mortality is not always close. For example, people aged 60 or more accounted for 70% of deaths in Peru, but only 12.5% of its total population.
There are indications that the quality of COVID-19 mortality data in many countries is not all that it could be, and there are particular causes for concern in some LMICs. The Mexican government has a COVID-19 data portal, with clearly presented and accessible information (8). However, recent media reports have claim that a large number of COVID-19 deaths in Mexico might have gone unreported(9).
Similar concerns have been raised with reference to other LMICs, including a study indicating that official COVID-19 mortality data in Indonesia could represent only a third of true levels(10). It has been reported that Peru’s official data on COVID-9 mortality up to 12 July might have captured only around a fifth of total excess mortality and registered deaths, and that under-reporting was higher for people at older ages(11). Taken together, these studies and reports indicate that the official data presented in Table 1 may substantially misrepresent the reality of the pandemic.
It is easy to criticise governments about the poor quality of COVID-19 mortality data. However, we must not ignore how challenging the collection and compilation of good data must be. Diagnosing cause of death is not easy at the best of times and cause of death data were very incomplete in most LMICs even before the pandemic hit. Diagnosis is especially challenging for people at very old ages, due to higher frequency of multiple health conditions and a tendency to view these events as simply dying of old age(12).
In the face of these many problems, how can we eventually get a clearer view of how the pandemic is affecting people at different ages? The best solution would be to improve reporting and diagnosis, but it may not be feasible to substantively improve these in the context of the pandemic. Local, downstream data may provide more reliable, if piecemeal, pictures and be used to validate national sources. For example, a study of burials in the Brazilian city of Manaus over a 10 day period found the number was four times higher than corresponding periods in previous years(13). Of these, 1,230 deaths, just 14 were reported as caused by COVID-19. Similarly, estimates of excess all-cause mortality can also be used to validate official COVID-19 mortality and can also reveal indirect mortality effects of the pandemic. Finally, simple models of COVID-19 mortality offer a useful alternative to reported data and are now widely available for LMICs(14).
We need good data about how COVID-19 is affecting people at different ages. Since older people are the most-at-risk group, any general response to the pandemic has to pay special attention to them, even if only to manage pressures on health services. Without data on older people, we cannot assess whether they are being fairly treated and whether preventive actions are reducing or even increasing their risk of dying. Amidst widespread concerns about explicit and implicit ageism in COVID-19 policy, there is a need to keep a close eye on what is really going on.
Ultimately, improved reporting on COVID-19 mortality in general, as well as by age groups will be a matter of political will, both at the global level and in individual LMICs. Tackling this would provide an invaluable public health legacy of enhanced mortality and cause of death data over future decades.
References
1. Albone R. HIV statistics and targets exclude older people putting millions of people at risk. | HelpAge International [Internet]. HelpAge International. 2011 [cited 2020 Nov 18]. Available from: https://www.helpage.org/blogs/rachel-albone-667/hiv-statistics-and-targetsexclude-older-people-putting-millions-of-people-at-risk-285/
2. Lloyd-Sherlock P, Ebrahim S, McKee M, James Prince M. Institutional ageism in global health policy. BMJ [Internet]. 2016 [cited 2020 Nov 18];354. Available from: http://www.who.
3. Magnani C, Azzolina D, Gallo E, Ferrante D, Gregori D. How large was the mortality increase directly and indirectly caused by the COVID-19 epidemic? An analysis on all-causes mortality data in Italy. Int J Environ Res Public Health [Internet]. 2020 May 2 [cited 2020 Nov 18];17(10). Available from: /pmc/articles/PMC7277828/?report=abstract
4. WHO. WHO Coronavirus Disease (COVID-19) Dashboard | WHO Coronavirus Disease (COVID-19) Dashboard [Internet]. 2020 [cited 2020 Nov 18]. Available from: https://covid19.who.int/
5. Johns Hopkins Coronavirus Resource Center. COVID-19 Map - Johns Hopkins Coronavirus Resource Center [Internet]. 2020 [cited 2020 Nov 18]. Available from: https://coronavirus.jhu.edu/map.html
6. Lloyd-Sherlock P, Ebrahim S, Geffen L, McKee M. Bearing the brunt of covid-19: Older people in low and middle income countries. BMJ [Internet]. 2020;368(March):1–2. Available from: http://dx.doi.org/doi:10.1136/bmj.m1052
7. Population Division - United Nations. World Population Prospects 2019 [Internet]. 2019 [cited 2020 Nov 18]. Available from: https://population.un.org/wpp/Download/Standard/Population/
8. Gobierno de México. COVID-19 Tablero México - CONACYT - CentroGeo - GeoInt - DataLab [Internet]. 2020 [cited 2020 Nov 18]. Available from: https://datos.covid-19.conacyt.mx/
9. Dyer O. Covid-19: Mexico acknowledges 50 000 more deaths than official figures show. BMJ [Internet]. 2020 Oct 29 [cited 2020 Nov 18];371:m4182. Available from: http://dx.doi.org/10.1136/bmj.m4182
10. Mulyanto R. Data science project reveals Indonesia Covid-19 death toll three times higher than official tally. The Telegraph [Internet]. 2020 Aug 17 [cited 2020 Nov 18]; Available from: https://www.telegraph.co.uk/global-health/science-and-disease/data-science-project-reveals-indonesia-covid-19-death-toll-three/
11. Sempé L, Lloyd-Sherlock P. Estimating excess of deaths during COVID-19 pandemics - A step-by-step tutorial and guidance. 2020 Jul. Report No.: 01.
12. Miki J, Rampatige R, Richards N, Adair T, Cortez-Escalante J, Vargas-Herrera J. Saving lives through certifying deaths: Assessing the impact of two interventions to improve cause of death data in Perú. BMC Public Health. 2018;18(1):1–11.
13. Orellana JDY, da Cunha GM, Marrero L, Horta BL, da Costa Leite I. Explosion in mortality in the Amazonian epicenter of the COVID-19 epidemic. Cad Saude Publica [Internet]. 2020 Jan 1 [cited 2020 Nov 18];36(7). Available from: http://www2.datasus.gov.br
14. Lloyd-Sherlock P. Estimating the impact of COVID-19 on older people in LMICs: the PICHM calculator [Internet]. 2020 [cited 2020 Nov 18]. Available from: https://corona-older.com/2020/09/26/estimating-the-impact-of-covid-19-on-older-people-in-lmics-the-pichm-calculator/
15. Riffe T, Acosta E, The COVerAGE-DB team. COVeAGE-DB: A database of age-structured COVID-19 cases and deaths. medRxiv [Internet]. 2020 Oct 30 [cited 2020 Nov 18];2020.09.18.20197228. Available from: https://www.medrxiv.org/content/early/2020/09/23/2020.09.18.20197228
Table 1. Reported COVID-19 deaths for selected countries, total population and people aged 60 and over (most recent available date).
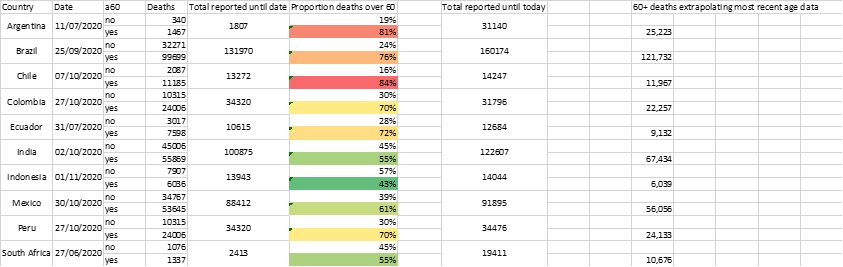
Source: COVeAGE-DB: A database of age-structured COVID-19 cases and deaths (15).
1 Data are available for some LMICs with lower COVID-19 mortality. For example, in Jamaica where people aged 60+ accounted for 69.8% of the 205 COVID-19 deaths reported by 30 October 2020 (https://jamcovid19.moh.gov.jm/).

